Do you leak when you cough, sneeze or laugh?
Do you leak with exercise e.g. running, jumping, skipping?
Or do you leak when standing up from a chair?
1 in 3 women have one or more of these complaints, and a lot of these women think that this is normal or just what happens after giving birth. However, although this seems common it is NOT NORMAL and it can be treated. All of these symptoms are related to stress urinary incontinence which is defined by “The of involuntary loss of urine on effort or physical exertion, or on sneezing or coughing” (IUGA/ICS 2010 terminology report).
There is good evidence that shows that pelvic floor physiotherapy can help with urinary incontinence and prolapse and can lessen the effects of childbirth and menopause on the pelvic floor.

There are two main reasons that stress urinary incontinence occurs and if you read our Pelvic Organ Prolapse blog post you may find that there are similarities in relation to the dysfunction of the pelvic floor muscles and fascia.
1. Urethral support deficiency: Refers to structures that provide a supportive layer upon which the urethra rests e.g. anterior vagina, endopelvic fascia and levator ani (deep pelvic floor). If any of the structures supporting the urethra become damaged, e.g. during child birth, the urethra can move lower and not sit in its usual position. This will change the ability of pressures to transmit equally to the bladder and upper urethra in times of increased intra-abdominal pressure e.g. cough, sneeze, lift, therefore increasing the chance of SUI.
2. Intrinsic sphincter deficiency (ISD): The dysfunction of urethral elements that result in overall urethral closure pressure i.e. volume and structure of urethral muscle, nerve innervation, sphincter facilitation, vascular closure pressure, urethral wall structure and elasticity.
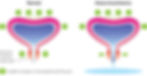

Management of Stress Urinary Incontinence:
1. The Knack: Squeeze and lift action of Levator Ani (pelvic floor muscles) provides counteraction to downward intra-abdominal pressure, closing compression of urethra.
Teaching the knack is predominantly about improving coordination of the pelvic floor muscles.
2. Pelvic floor strengthening: Permanent changes to muscle morphology, increased resting tone, increased cross-sectional area of the muscle.
3. Other
o Weight loss
o Oestrogen replacement
o Artificial supports of urethra e.g. use of a pessary. See our pelvic organ prolapse blog post for more information.
A pelvic floor physiotherapist is an important part of the multi-disciplinary team managing bladder and bowel health, sexual difficulties and pelvic pain. Women should not have to put up with incontinence, pelvic pain or discomfort. Get in contact with us today on (02) 4454 2309.
